Mydriasis, or pupillary dilation, is defined as an increase in pupil diameter beyond 4 mm—corresponding to more than 33% of the iris diameter—under daylight or standard artificial lighting conditions. This finding may result from several underlying mechanisms, including:
- Paralysis of the pupillary sphincter secondary to parasympathetic nerve injury, characterized by absence of the light reflex and lack of response to pilocarpine.
- Irritation or hyperactivity of sympathetic innervation, producing spastic mydriasis in which the pupil retains reactivity to light.
- Impaired function of the pupillary sphincter due to dysfunction of afferent pupillary pathways, and less commonly mesencephalic internuncial neurons, in which pharmacologic stimulation with pilocarpine induces pupillary constriction.
Chronic pupillary dilation is predominantly mediated by sustained sympathetic nervous system activity.
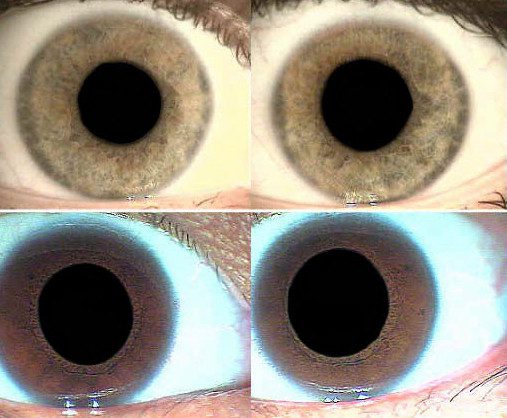
Physiological Mydriasis
Physiological mydriasis may occur under conditions similar to those associated with physiological miosis and can result from a variety of normal reflex and emotional responses, including:
Sexual arousal, with pupillary differences of up to 0.25 mm, more frequently observed in individuals with light-colored irides.
Pain, typically mediated by increased catecholamine (adrenaline) release.
Emotional stimuli such as pleasure, fear, irritation, anger, heightened attention, or desire.
Vestibulo-pupillary reflexes, characterized by sustained pupil dilation following brief, transient constrictions due to vestibular system stimulation.
Cochleo-pupillary reflexes.
The promortal phase, occurring at the time of death and during the first two to three hours postmortem.
Pathological Mydriasis
Pathological mydriasis may arise from diverse etiological and pathogenetic mechanisms, including:
Comatose states, such as thyrotoxic, epileptic, eclamptic, hepatic, and hypochloremic coma.
Endocrine disorders, including Graves’ disease.
Severe infectious processes, for example botulism.
Chronic or severe pain syndromes.
Meningeal irritation, including manifestations such as Flatau’s sign.
Visceral disorders associated with hyperthermia, hypertensive crises, or dyspnea.
Toxic exposures, including alcohol, narcotic hallucinogens, carbon disulfide, and dinitrophenol.
Pharmacologic effects, particularly from adrenomimetic agents and anticholinergic drugs (e.g., novocaine).
Psychogenic reactions, including hysterical episodes (e.g., Raedlich’s sign).
Associated systemic conditions, such as adrenal exhaustion, urinary tract pathology, bronchial disorders, and gastrointestinal dysfunction.
Diagnostic Considerations
Unilateral mydriasis is of particular diagnostic significance in the evaluation of central nervous system pathology and may be observed in syndromes involving optic nerve lesions, oculomotor nerve paralysis, and various post-traumatic states.
While unilateral miosis or mydriasis occurring as part of a broader clinical syndrome is typically straightforward to diagnose, the differential diagnosis of isolated unilateral pupillary abnormalities can be challenging. In such cases, pharmacological testing with agents such as adrenaline or homatropine may be required to clarify the underlying mechanism.


